Over my 20-year career as a medical officer and practitioner, I’ve observed few health conditions wreak as much far-reaching damage on patient well-being and quality of life as stress.
Six in ten of us1 experience high levels of stress, and young people tend to feel it worse. In fact, Cigna Healthcare’s latest assessment of global wellbeing shows how today’s main driver of stress – the cost-of-living crisis – is having an unprecedented and disproportionate impact on younger generations.
The consequences of this global state of mind are worrying. Earlier onset of chronic disease, a greater burden of physical illness, more hospitalizations for potentially preventable reasons, and in the most severe cases, premature death.2 It’s a troubling fact that people with mental illnesses live anywhere between 10 to 20 years less than those without.
In light of these facts, there can be little doubt that stress and its toll on our bodies is one of the world’s most pressing health issues. Let’s talk about it.
The Relationship Between Mental Health and Physical Health
A few years ago, I embarked on a research project exploring the connection between mental health and physical illnesses. We wanted to understand if individuals with pre- existing mental health issues would face more significant challenges when dealing with a physical ailment, and whether they would require extra support to return to good health from major treatment or ill-health, like hip surgery or pneumonia.
It’s well known that many, if not all physical health problems come with a psychological dimension3, and those who suffer long-term physical health conditions are susceptible to severe mental health problems4, such as depression or anxiety.
But our task was the opposite: to quantify the financial impact so that people could really appreciate the link mental ill-health and general physical well-being. That is, how investing in mental health benefits can help to counteract physical ailments.
The results of our study were surprising. Despite appreciating the significant economic toll5 of mental ill-health on physical productivity, many companies and HR departments still struggled to grasp the interconnectedness of the two elements of well-being. Instead, they tended to treat mental health as a separate issue, overlooking its influence on physical health.
The conclusions were obvious: addressing mental health alongside physical conditions is crucial. For example, treating a work-related back injury will require physiotherapy but may also necessitate counselling services, via health insurance or benefits packages, to treat the underlying stress or tension contributing to the orthopedic or muscular strain. I spoke with clinical experts at Ellipsis Health who partnered with Cigna Healthcare on StressWaves, a free tool that Cigna Healthcare offers to support emotional wellbeing globally. Dr. Michael Aratow, Co-Founder and Chief Medical Officer at Ellipsis Health said, “We have to change our fundamental view of health to encompass a holistic viewpoint. We think nothing of going to the gym and measuring our performance to improve our physical health, so should we think nothing of utilizing tools to measure and improve our mental health.”
Stress: The Misunderstood Link Between Mental and Physical Health
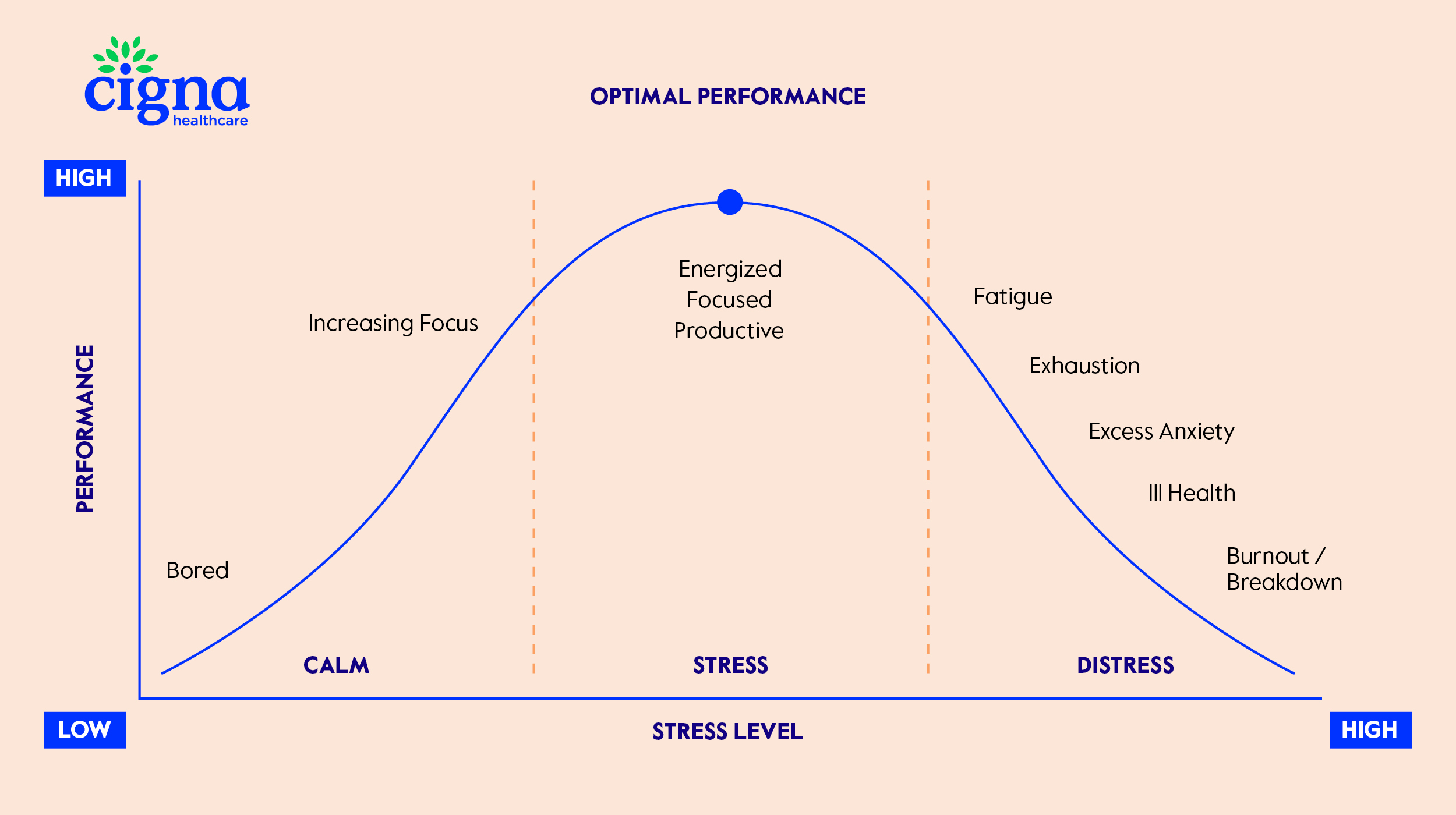
Stress is both a global problem and a fundamental part of life, for better and worse. A small amount of acute stress is to be expected and can even be good6, as it helps us with decision-making and performing daily activities. The trouble starts when stress persists.
Too much or chronic stress can overwhelm our mind and body, causing a number of physical health issues7, from increased vulnerability to viral infections, to headaches, fatigue, insomnia, overeating, and gastrointestinal problems. It also leads to life-threatening conditions8, such as hypertension, heart disease, Type II diabetes, obesity and metabolic syndrome, as well as a heightened risk of substance abuse.
Although the link between stress and overall physical well-being may be obvious to healthcare professionals, patients often neglect symptoms or delay diagnosis due to fundamental misconceptions about the nature of stress and mental health.
In many instances, people first try to cure the physical symptoms, without recognizing the social or personal determinants of stress as the root cause. For example, a patient may go for dozens of physiotherapy sessions to treat their back pain and achieve limited relief as they have not acknowledged their pain as induced by work9 or social or cultural10 stressors.
But the consequences of our collective inability to talk about stress early are felt by all.
It’s estimated that chronic stress causes much greater health service utilization11, more visits to the family doctor, counsellor, specialists and hospitals, exacerbating the already huge demand on our healthcare systems.
The demand that physical ailments inevitably place on health providers due to untreated underlying psychological conditions is an issue that companies like Cigna Healthcare are constantly seeking to address through better, more preventative and holistic well-being benefits.
Chronic inflammation: How Physical Health Conditions Affect Mental Health
In 2019, my research explored the correlation between common physical illnesses and mental health. Specifically, we identified connections between conditions like eating disorders and chronic gastritis, which are both linked to chronic inflammation. This inflammation, often triggered by an unhealthy diet, lack of exercise or chronic stress, not only heightens the risks of diabetes and obesity but also acts as a defense against infections and injuries.
Interestingly, however, recent years have revealed a twist in our understanding of inflammation. Rather than just serving a protective purpose, we now know that inflammation plays a role12 in the genesis of certain types of depression.
Notably, individuals grappling with inflammatory ailments tend to be more susceptible to depression than those dealing with non-inflammatory conditions like heart disease. This susceptibility escalates alongside the level of inflammation, then amplifying the risk of depression in a vicious cycle.preciating inflammation's complex duality – acting as both a protector and a potential underminer of our mental health – is going to be increasingly crucial to our collective understanding of how physical health and mental well-being are intricately linked and play equal roles in holistic well-being.
How can I approach my health holistically?
Here are a few key habits that will help you stay on top of your mental and physical health:
- See your doctor: This may be challenging for some, as recent years have made it harder to keep up sustainable and preventable treatment despite increasing awareness about stress and mental health. During COVID-19, regular GP and family doctor visits fell disastrously13, and in the wake of the pandemic we have seen issues with access and affordability. Nevertheless, seeing a doctor regularly is vital.
In acutely stressful situations, up to six sessions with a mental health professional or specialist clinician might be enough for you to cope better and get on top of any emerging physical issues. But if you’re experiencing chronic stress over an extended period, you will likely need more systematic support.
- Manage your working hours: With today’s ‘always on’ culture it’s incredibly easy for work to dominate every waking hour. In a study last year, we found that nearly all employees globally were showing signs of burnout, a major cause of mental ill-health, which can manifest itself physically as back pain or other conditions. While everyone’s working style is different, it’s important to manage your boundaries between work and personal time.
- Practice Mindfulness: As Ellipsis Health’s Michelle Hoy, SVP and an experienced therapist, recommends, “try breath work, meditation, yoga, or any number of other practices that will assist you in connecting to your body and quieting your mind, allowing you to become more grounded and calm.”
- Speak to your family and friends: In 2020, around 78% of people14 globally who suffered anxiety or depression actively turned to family or friends to talk about their condition, leaving a significant shortfall of people across the globe who stayed silent. The value of talking openly about our mental health cannot be understated, and our first port of call is usually our family and friends.
- Stay active: The role physical exercise plays in supporting a healthy mind and body15 is becoming more and more apparent. Movement helps keep you balanced and in shape – both in mind, body and mood.
Looking towards a new approach to holistic and preventative healthcare
The connections between mental and physical health are undeniable and profound.
Chronic stress and mental illnesses silently impose a heavy toll on physical well-being, costing trillions to the global economy and stealing precious years of life from billions of people.
Promisingly, however, the interplay between mental and physical health has gone from being an obscure corner of research to a central field of medical attention and even popular awareness. And as I look to the future of medicine, it is exciting to see the mind-body connection emerging as the next significant area of discovery for effective, holistic, and preventative healthcare.
But, for this knowledge to improve our everyday quality of life, it is essential that we pay attention to how stress, inflammation, exercise, sleep, diet16, and social connections17 all interact, and that patients and clinicians pursue holistic healthcare strategies that reflect this link.
Of course, one of the most important elements of this new approach will be our ability to talk openly with our doctors, friends, and family about how we are doing physically, mentally holistically. Be brave and ask someone you know how they are doing emotionally or share your recent emotional state to start a conversation. As Dr. Aratow suggests, “Language is a powerful force, and we have to get to a point where the word ‘health’ means both physical and mental well-being, and when we are there, the stigma fades away and the tides can be turned on the decades long mental health epidemic affecting the entire world.”
1. Majority of adults report experiencing high levels of stress in past year. https://www.ipsos.com/en-us/news-polls/world-mental-health-day-monitor-2022. Published October 5, 2022.
2. JAMA Network. Mortality in Mental Disorders and Global Disease Burden Implications. https://jamanetwork.com/journals/jamapsychiatry/fullarticle/2110027. Published April 2015.
3. The King’s Fund. Bringing together physical and mental health. https://www.kingsfund.org.uk/sites/default/files/field/field_publication_file/Bringing-together-Kings-Fund-March-2016_1.pdf. Published March 2016.
4. The Lancet. Epidemiology of multimorbidity and implications for health care, research, and medical education: a cross-sectional study. https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(12)60240-2/fulltext. Published May 10, 2012.
5. The Lancet Global Health. Mental health matters. https://www.thelancet.com/journals/langlo/article/PIIS2214-109X(20)30432-0/fulltext. Published November 2020.
6. World Health Organization. Stress. https://www.who.int/news-room/questions-and-answers/item/stress. Published February 21, 2023.
7. Cigna Healthcare. The Effects of Stress and Their Impact on Your Health. https://www.cigna.com/knowledge-center/effects-of-stress-and-their-impact-on-your-health. Last accessed November 17, 2023.
8. Yale Medicine. Chronic stress. https://www.yalemedicine.org/conditions/stress-disorder. Last accessed November 17, 2023.
9. BMC Public Health. How are social stressors at work related to well-being and health? A systematic review and meta-analysis. https://bmcpublichealth.biomedcentral.com/articles/10.1186/s12889-021-10894-7. Published May 10, 2021.
10. National Library of Medicine. Stress and its Social Determinants – A Qualitative Study Reflecting the Perceptions of a Select Small Group of the Public in Sri Lanka. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6970305/. Published January 6, 2020.
11. Cigna Healthcare. Chronic Stress: Are we Reaching Health System Burn out? https://www.cignaglobal.com/static/docs/pdf/cigna-asia-care-report-18-nov.pdf. Published November 2019.
12. National Library of Medicine. The Role of Inflammation in Depression and Fatigue. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6658985/. Published July 19, 2019.
13. EurekAlert. Study shows diagnoses of common conditions at family doctor halved during COVID-19 lockdown. https://www.eurekalert.org/news-releases/664166. Published September 23, 2020.
14. Our World in Data. Dealt with anxiety or depression by talking to friends or family, 2020. https://ourworldindata.org/grapher/dealt-with-anxiety-depression-friends-family?tab=table. Last accessed November 17, 2023.
15. Nature Mental Health. Major depression, physical health and molecular senescence markers abnormalities. https://www.nature.com/articles/s44220-023-00033-z. Published March 22, 2023.
16. National Library of Medicine. Healthy Eating, Physical Activity, and Sleep Hygiene (HEPAS) as the Winning Triad for Sustaining Physical and Mental Health in Patients at Risk for or with Neuropsychiatric Disorders: Considerations for Clinical Practice. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6955623/. Published January 8, 2020.
17. Springer Nature. Exploring the relationship between social connectedness and mental wellbeing: the mediating role of psychological resilience among adults in Azerbaijan. https://link.springer.com/article/10.1007/s44202-023-00080-8. Published June 26, 2023.
Offered by Cigna Health and Life Insurance Company or its affiliates.
This information is for educational purposes only. It's not medical advice. Always consult with your health care provider for appropriate examinations, treatment and health care recommendations.
This article serves only as a reference and is intended for informational purposes only. Nothing in this article constitutes legal, tax, financial planning, health or medical advice including diagnosis or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. References to third-party organizations or companies, and/or their products, processes or services, do not constitute an endorsement or warranty thereof. Products and services may not be available in all jurisdictions and are expressly excluded where prohibited by applicable law. All group insurance policies and health benefit plans contain exclusions and limitations. For costs and details of coverage, contact a Cigna Healthcare representative.
Product availability may vary by location and plan type and is subject to change. Products may not be available in all jurisdictions and are excluded where prohibited by law. All group health insurance policies and health benefit plans contain exclusions and limitations. For costs and details of coverage, review your plan documents or contact a Cigna Healthcare representative. Cigna Healthcare products and services are provided exclusively by or through operating subsidiaries of The Cigna Group, including Cigna Health and Life Insurance Company, Cigna Life Insurance Company of Canada, Cigna Global Insurance Company Limited, Evernorth Care Solutions, Inc., and Evernorth Behavioral Health, Inc. The Cigna Healthcare name, logo, and other Cigna marks are owned by Cigna Intellectual Property, Inc., licensed for use by The Cigna Group and its operating subsidiaries. “Cigna Healthcare” refers to The Cigna Group and/or its subsidiaries and affiliates. The information on this site is only a general description of benefits. All insurance policies and group benefit plans contain exclusions and limitations.
Cigna Healthcare products and services are provided exclusively by or through operating subsidiaries of The Cigna Group, including Cigna Health and Life Insurance Company, Life Insurance Company of North America, Cigna Global Insurance Company Limited, Evernorth Care Solutions, Inc., Evernorth Behavioral Health, Inc., or through their affiliates and contracted companies.